The Left Ventricular Assist Device (LVAD) is a revolutionary device that has reduced the need for heart transplants worldwide. The LVAD is used in patients with severely weakened heart muscle. It is a pump that is implanted into the Heart, and can generate an amount of blood flow which is equivalent to the amount the normal heart pumps. Some patients can recover enough function after the LVAD to return to work.
What is a Left Ventricular Assist Device (LVAD)?
A Ventricular Assist Device (VAD), or Mechanical Circulatory Support Device, is a device that assists your heart in pumping blood from the lower chambers (ventricles) to the rest of the body. It is surgically implanted, either temporarily while you wait for a transplant, or permanently to help your heart produce enough blood for the body. Although the VAD can be placed on one or both ventricles, it is most commonly implanted.
How does the LVAD work?
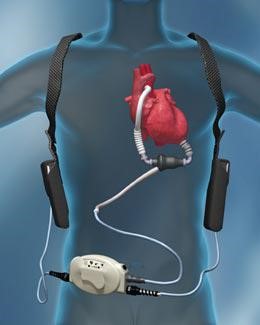
- The LVAD pump unit is surgically implanted into the apex of the heart. A tube connected to the device collects the blood from the heart and delivers it to the Aorta.
- The pump unit is connected to a driveline and a control system. The driveline passes from the unit, through the abdominal skin, to the control system outside your body. This system helps regulate the pump and provides you with messages to help operate the unit.
Who can have an LVAD?
If you fall into any of these categories, you may be recommended by your doctor for an LVAD implantation:
- If you are waiting for a heart transplant – A temporary VAD could be used while awaiting a suitable donor for your transplant. The VAD will assist in pumping blood through your body until the replacement heart arrives.
- You cannot have a heart transplant – Due to reasons such as age or other factors, a permanent VAD can be used to improve the quality of your life. Also known as Destination Therapy, this procedure can help those with heart failure and other issues, that cannot be treated using a transplant due to underlying conditions.
- You have temporary heart failure – A VAD may be temporarily implanted to help your heart recover in cases of a temporary failure. Once it is healthy enough to function normally, the VAD will be removed.
Getting a VAD however depends on the following factors:
- The severity of your heart failure
- Other underlying medical conditions you may have
- How well do the main chambers of the heart work
- Ability to safely use blood thinners
- The social support of your family and friends
- Your personal mental health and ability to take care of a VAD
What are the benefits of LVAD?
An LVAD increases the blood flow to the body, in turn improving other related functions in the body. An LVAD can greatly improve the function of the kidneys, liver, brains and other organs, while also increasing your strength and ability to participate in activities. Implantation and proper functioning of an LVAD can also provide you with a greater life expectancy, a better quality of life and even reduces your symptoms of heart failure.
What are the risks of LVAD?
There are, of course, risks associated with the implantation of an LVAD. They include:
- Bleeding – any surgery can increase your risk of bleeding.
- Blood clots – as blood moves through the LVAD, blood clots may form. These can slow or block blood flow, causing improper functioning of the device that can lead to strokes or heart attacks.
- Infection – as the power source and control unit for the LVAD is located outside the body, and are connected to the pump unit through a wire passing through your abdominal skin, there’s an increased risk of germs getting into the area, causing an infection at the site or in your blood.
- Device problems – An LVAD may sometimes stop working properly after it’s implanted. For instance, the device may not pump blood properly or the power supply could fail. These issues will require immediate medical attention and may lead to the replacement of the device.
- Right heart failure – Since an LVAD is implanted in the left ventricle, the right ventricle may become too weak to handle the increased blood flow in the left. A temporary pump may be then needed to assist the right side as well, or other treatments such as medication or therapies may be needed to help the right ventricle match up to the left.
How do I prepare before and after the LVAD implantation?
BEFORE
- Once finalised, the doctor will clarify the details of the implantation with you and assist you throughout the procedure.
- Before the surgery, you will be required to stop eating and drinking for several hours, usually specified by the doctor/treatment team.
- If you are on any other medications, those may be monitored and your doctor will let you know the medications that can or cannot be taken prior to the surgery.
- You will likely be asked to avoid wearing contact lenses, dentures, eyeglasses, jewellery and/or nail polish for the procedure.
AFTER
- You will be admitted to intensive care post-surgery, where your doctor/treatment team can adjust and administer the right aftercare treatments for your heart, while also ensuring no complications occur.
- While in intensive care, you will likely receive fluids and medication through an IV, and might also have tubes connected to drain urine from the bladder as well as fluid and blood from the chest/heart. You may also be administered antibiotics to prevent infections, as well as blood thinners to prevent blood clots.
- Immediately after the surgery, your lungs may not work properly for a few days. A ventilator may be given to you until you can breathe on your own.
- After a few days in the ICU, you’ll likely be shifted to a regular ward. Depending on your recovery rate and your health conditions, you will be asked to stay longer or be discharged in a few days. During your time in the hospital, you will be assisted by physical therapists and other specialists to get more active and stronger. They will help you sit up, get out of bed and walk. If you require more time to regain your strength, you may be recommended a short stay at a rehabilitation facility.
- Your family will also be informed about the aftercare and support required from their side. They will be educated on how to identify signs/symptoms of an infection, what to do if the device isn’t working properly, how to keep the incision site and cords clean, how to shower without damaging the device, and how to travel with the VAD, ways to decrease stress and anxiety for the patient as well as when the patient can safely return to daily life activities.
**The above information is for general knowledge only and does not constitute medical advice. Please consult a doctor if you have any questions or symptoms.
