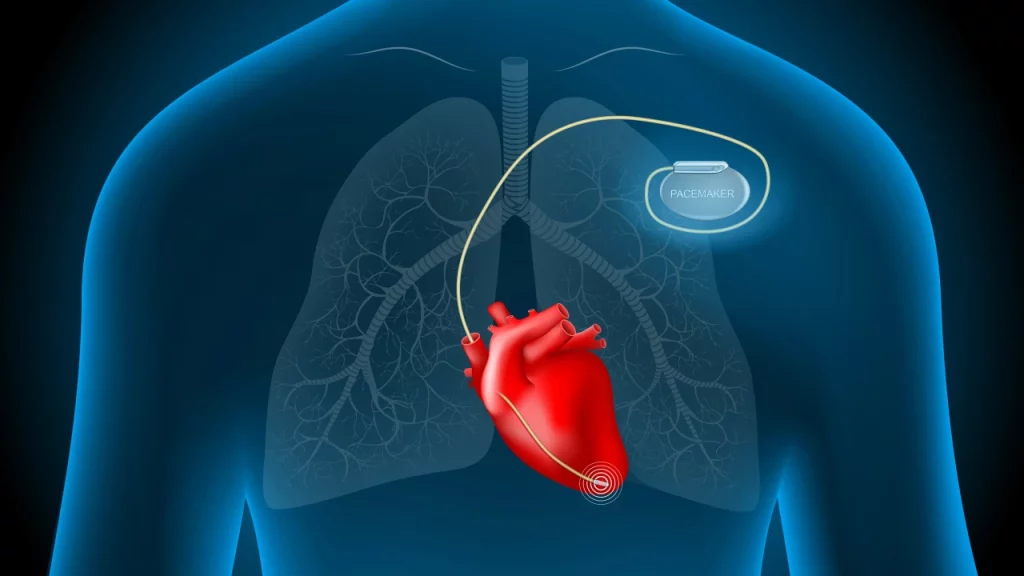
Pacemaker & Cardiac Device Implantation
A Pacemaker is an Electronic device with a Power source that is implanted in the patient’s body, usually in the Upper Chest (on the side opposite the dominant hand). It is usually implanted when the patient’s own internal heart rate is too slow, causing symptoms such as giddiness, fatigue, and even fainting. A shielded wire is connected to the Pacemaker and is secured inside the heart chamber, so as to detect the intrinsic heartbeat, and if required, deliver a pulse of energy to the heart muscle to stimulate it to beat.
More advanced Pacemakers can deliver a high energy electrical shock internally so as to terminate an abnormal heart rhythm and restore a normal heartbeat.
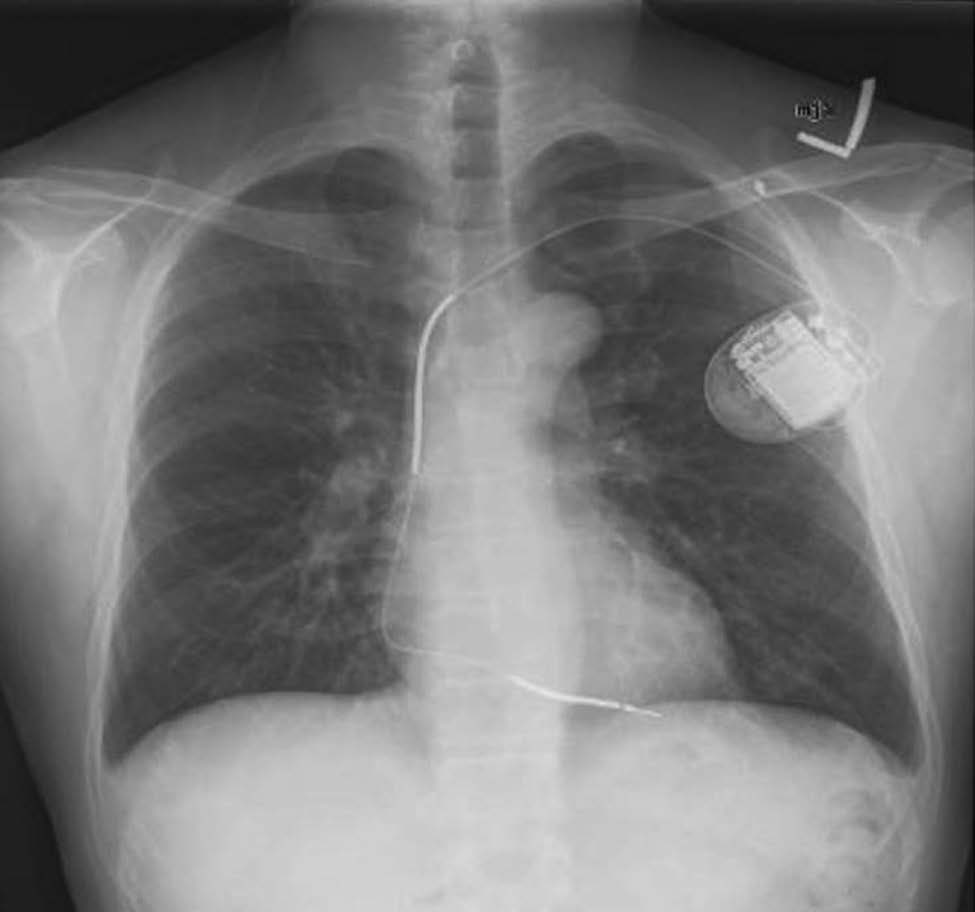
What is a pacemaker?
A pacemaker, also known as a Cardiac Pacing Device, is a small apparatus placed or implanted into the chest to help regulate one’s heartbeat. Requiring a surgical installation, this device is often used to make sure that the heart isn’t beating too slowly.
More advanced Pacemakers can deliver a high energy electrical shock internally to terminate an abnormal heart rhythm and restore a normal heartbeat.
Why I may need pacemaker implantation?
- A pacemaker is implanted to help regulate and control your heartbeat. If you have been diagnosed with a slow heartbeat (bradycardia) after a heart attack, surgery or a medication overdose, a temporary pacemaker can help you recover. A more permanent one may be implanted in cases wherein the patient has a chronically slow or irregular heartbeat and/or heart failure.
- Depending on the severity and complexity of your condition, different kinds of pacemakers can be used, each serving a separate function:
- Single Chamber Pacemaker – this usually sends electrical impulses to one part of the heart, namely the right ventricle.
- Dual Chamber Pacemaker – this usually sends electrical impulses to both the right atrium and ventricle, to correct and regulate the timing of their contractions.
- Biventricular Pacemaker – as the name suggests, this device sends impulses to both the left and right ventricles to regulate a proper heartbeat. This is used in Cardiac Resynchronization Therapy (Biventricular Pacing), which helps correct conditions such as heart failures or other complex heart problems.
What is the risk of pacemaker implantation?
Risks or complications related to a pacemaker surgery are uncommon for the most part, but they could include:
- Infections near the area in the heart where the device is implanted.
- Swelling, bruising or bleeding near the pacemaker implantation; especially if the patient consumes blood thinner medication.
- Blood clots, or Thromboembolisms, near the pacemaker region.
- Damage to the blood vessels or nerves near the pacemaker.
- A collapsed lung, or Pneumothorax.
- Blood accumulation in the cavity between the lung and the chest wall is known as Hemothorax.
- Movement or shifting of the pacemaker could lead to cardiac perforations (this is a rare occurrence).
What are the necessary precautions required after Pacemaker Implantation?
- You will likely be admitted to the hospital post-surgery, as the device gets programmed to match your heart’s pace. Your doctor may advise you to avoid vigorous activity or heavy weight lifting for about a month, as well as avoid applying pressure to the pacemaker region. If you experience pain in the region, it is advised to consult your doctor on the type of painkillers that can or cannot be consumed.
- Once the pacemaker is implanted and well-adjusted, there are a few things that the patient is to keep in mind at all times, to ensure the proper functioning of the device without any mechanical complications:
-
- Cellphones – People with pacemaker implants are advised to not have their mobile devices in their shirt pockets, and are also expected to keep them at least 6 inches away from the pacemaker. It is safe to attend calls, but do note that calls must be answered using the ear farther away from the pacemaker.
- Security Systems – During airport security checks, the metal in the pacemaker could sound the alarms but is not harmful to the functioning of the device. It is always a safer option to carry an ID stating that you have a pacemaker, to ensure a smooth security checking.
- Medical Equipment – No matter what the treatment it is that you are opting for, always make sure that your doctors/dentists know about your pacemaker. Certain medical treatments and equipment can interfere with the pacemaker, such as Magnetic Resonance Imaging (MRI) scan, CT scans, Cancer Radiation treatment, Electrocautery to control bleeding during surgery, as well as Shock Wave Lithotripsy used for treating large kidney or gall stones.
- Do note that it is wise to have your pacemaker checked every 3 to 6 months, or if you experience sudden weight gain, puffy ankles or legs, or even dizziness.
- Your pacemaker should last anywhere from 5 to 15 years. Upon expiry or any faults, your doctor will have to surgically replace the battery, which is often a safer and quicker process.